Requirement of Active and Passive Air Sampling in Controlled Areas
Air sampling is a mandatory procedure to be followed in pharmaceuticals to produce the contamination free quality product.
 |
| Contamination Of Products |
However, air is another key source of contamination that most pharmaceutical facilities often ignore to take precaution from. Air particulate sampling or air monitoring is essential for Quality Control (QC) purposes especially in companies that manufacture pharmaceutical products in controlled areas or clean rooms with filtered air.
 |
| Bioburden |
The two main methods used to sample air are:
- Active air sampling/ monitoring
- Passive air sampling/ monitoring
1. Active Air Sampling
 |
| Active Air Sampling |
This method is sometimes referred to as pumped sampling where the air in the controlled area is kinetically monitored during manufacturing. What this means is, over a specific time period, a microbial air sampler is used to continuously force an already established volume of air to pass over a petri dish that serves as the artificial medium containing an agar nutrient based test media.
The Petri dishes containing medium are then removed from the air sampler and directly incubated. Incubation allows the collected culture that is the microorganisms such as bacteria, fungi etc to grow into visible colonies that can be easily identified and analyzed through counting. This gives a clear indicator of how many viable microorganisms are there per cubic meter of air.
Advantages
- It allows for both qualitative and quantitative analysis of the sample
- Allows for faster results as devices used for this method allow for a shorter sampling period such as 10 minutes
- Ideal for controlled areas as they tend to have a low microbial concentration
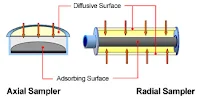 |
| Passive Air Sampling |
Just like in the active air sampling, the plates are then incubated to allow for the microorganisms that dropped onto the plates to grow into colonies that can accurately be analyzed.
Advantages
- For starters, the method is inexpensive as it does not require a lot of equipment
- Offers average contamination levels over long sampling periods that could range from hours to months
- No supervision is required during the sampling period
- Its affordability makes it easy to sample various contamination hotspots at once
As I mentioned above in active air sampling we determine bioburden in 1 cubic meter area and we sample 1000 liters of air by air sampler while in passive air sampling we determine that how much microbes settle in 90 mm diameter surface of any equipment exposed in controlled area.
A lot of pharmaceutical professionals have confusion in air sampling that which one should be done among both of samplings. But all regulatory guidelines say that it is mandatory to sample and analyze the clean room area by both methods of air sampling for a complete air quality assessment.

Comments
Post a Comment
If you have any doubts, please let me know